Hyperbaric Oxygen Therapy: The Complete Guide to HBOT in 2026
How it works, what it costs, the risks, and every option available to you
This guide is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician before starting any therapy.
What Is Hyperbaric Oxygen Therapy?
Hyperbaric oxygen therapy (HBOT) is a medical treatment where you breathe pure oxygen inside a pressurized hyperbaric chamber. The air pressure inside the chamber is raised to 1.5 to 3 times normal atmospheric pressure. This forces significantly more oxygen into your blood, tissues, and organs than normal breathing ever could.
At normal air pressure, your red blood cells carry about 97% of the oxygen your body uses. That sounds like plenty. But your plasma — the liquid part of your blood — carries very little oxygen under normal conditions.
Pressurized oxygen changes that. At 2.0 ATA (twice normal pressure), the oxygen in your plasma jumps by roughly 10 times. This extra oxygen reaches places red blood cells can’t — damaged tissue, swollen injuries, and areas with poor blood flow.
A Brief History
Doctors first used HBOT in the 1940s to treat deep-sea divers with decompression sickness (“the bends”). Navy doctors found that putting patients back under pressure in a sealed hyperbaric chamber stopped the dangerous nitrogen bubbles in their blood.
By the 1960s, researchers found that pressurized oxygen also sped up wound healing. Hospitals began using HBOT therapy for carbon monoxide poisoning, gas gangrene, and radiation injuries. Today, the FDA approves HBOT for 14 medical conditions [10]. Hundreds of clinics also use it for other, unapproved uses.
Who Uses HBOT Today?
- Wound healing patients — especially diabetic foot ulcers and radiation-damaged tissue
- Neurological conditions — TBI, stroke recovery, and other brain injuries (mostly off-label)
- Cognitive decline — early RCTs show improved attention and processing speed in adults 64+ [18]
- Chronic fatigue sufferers — early research suggests HBOT may reduce fatigue severity (Akarsu et al., 2013 [20])
- Anti-aging seekers — based on early research showing cells may age more slowly (Hachmo et al. / Efrati lab, 2020 [6])
- Athletes — seeking faster recovery from injuries and intense training
- Post-surgical patients — to support graft and flap survival
Benefits of Hyperbaric Oxygen Therapy
The benefits of hyperbaric oxygen therapy depend on what you are treating. For FDA-approved conditions like diabetic wounds, radiation injury, and decompression sickness, HBOT accelerates healing by flooding damaged tissue with oxygen under pressure. Research shows it promotes new blood vessel growth, mobilizes stem cells, and reduces inflammation. For off-label conditions like TBI, stroke recovery, and anti-aging, benefits are still being studied — early results are promising, but the evidence base is smaller.
How Your Body Responds
Three key mechanisms drive the effects of hyperbaric treatments:
At 2.4 ATA, plasma oxygen jumps from about 3 mL/L to over 50 mL/L — enough to keep tissue alive even without red blood cells.
Repeated sessions help grow new blood vessels in tissue that lacks oxygen. Studies show new tiny blood vessels forming after 20+ sessions.
One study found that a single session at 2.0 ATA doubled the stem cells moving through the blood. After 20 sessions, stem cell counts rose up to 8 times [19].
The Hyperoxic-Hypoxic Paradox
Dr. Shai Efrati’s team at Tel Aviv University found something surprising: it may not be the oxygen itself that triggers healing — it is the change between oxygen levels. In their method, patients inside a hyperbaric chamber breathe pure oxygen for 20 minutes, then switch to chamber air. Each switch tells the body to activate repair signals (HIF-1α) [14].
Their results were striking. In one small study (n=35), after 60 sessions, adults over 64 had telomeres that grew more than 20% longer and 37% fewer worn-out immune cells [6]. In simple terms, key markers of aging shifted in a direction researchers considered favorable.
What are telomeres? Think of the plastic tips on shoelaces. Telomeres are protective caps on the ends of your DNA strands. Every time a cell divides, those caps get a little shorter. When they get too short, the cell stops working well. Shorter telomeres are linked to aging and disease. Longer telomeres generally mean healthier, younger-acting cells.
What are senescent cells? When cells get old or damaged, some of them stop dividing but refuse to die. These “zombie” cells sit in your body, take up space, and release signals that cause swelling and damage to nearby healthy cells. Your immune system is supposed to clear them out, but as you age, more pile up.
The study protocol: Efrati’s team enrolled 35 healthy adults aged 64 and older. Each person completed 60 sessions over about 3 months. Sessions ran 5 days per week. Each session used a hyperbaric chamber pressurized to 2.0 ATA. Patients wore a mask that delivered pure oxygen for 20 minutes, then switched to breathing the chamber’s air for 5 minutes. This cycle repeated throughout each 90-minute session [6].
The results: Blood samples taken before and after the 60 sessions showed two clear changes. Telomere length on certain immune cells grew by over 20%. The number of senescent (worn-out) immune cells dropped by 37%. No drugs. No supplements. Just pressurized oxygen cycling [6].
Why does the cycling matter? This is the “Hyperoxic-Hypoxic Paradox” [14]. When you breathe pure oxygen and then switch to regular air, your body reads that drop as a low-oxygen event — even though the air pressure is still above normal. That sudden change flips on a protein called HIF-1α, which tells your body to grow new blood vessels, release stem cells, and clear out damaged cells. The key insight: constant high oxygen does not trigger this response. The switching does.
What this means: Efrati’s work suggests that the oxygen-cycling pattern — not just raw pressure — may be a core driver of HBOT’s anti-aging effects. This is still one study in a small group of healthy older adults. More research with larger groups is needed before drawing firm conclusions.
These are the reasons hyperbaric treatments work for certain conditions — and why it takes many sessions to see lasting results. Most treatment plans call for 20 to 40 sessions over several weeks.
FDA-Approved vs Off-Label Uses
This is where HBOT gets tricky. There is a big gap between what HBOT is proven to treat and what many clinics say it can treat. Knowing this gap protects your health and your wallet.
FDA-Approved Conditions
These uses are supported by decades of studies and strong proof:
For these 14 conditions, the evidence is strong. Insurance frequently covers treatment, and clinical protocols are well-established.
Off-Label Uses
Many clinics promote treatments beyond the FDA list. Here is what the evidence says today:
The bottom line: FDA-approved conditions have decades of evidence behind them. Popular off-label uses have much weaker evidence, and many clinics overstate the science. If a provider promises guaranteed results for an off-label condition, treat that as a red flag.
Types of Hyperbaric Systems
Not all hyperbaric chambers are equal. The pressure, the proof behind them, and the cost per session vary a lot. Knowing the differences helps you decide which option — if any — is right for you.
1. Clinical Hard-Shell Chambers (2.0–3.0 ATA)

These are the hyperbaric chambers used in hospitals and accredited clinics. They are large, rigid vessels — often made of steel or acrylic — capable of pressures up to 3.0 ATA (three times normal atmospheric pressure).
Clinical hyperbaric chambers come in two main types:
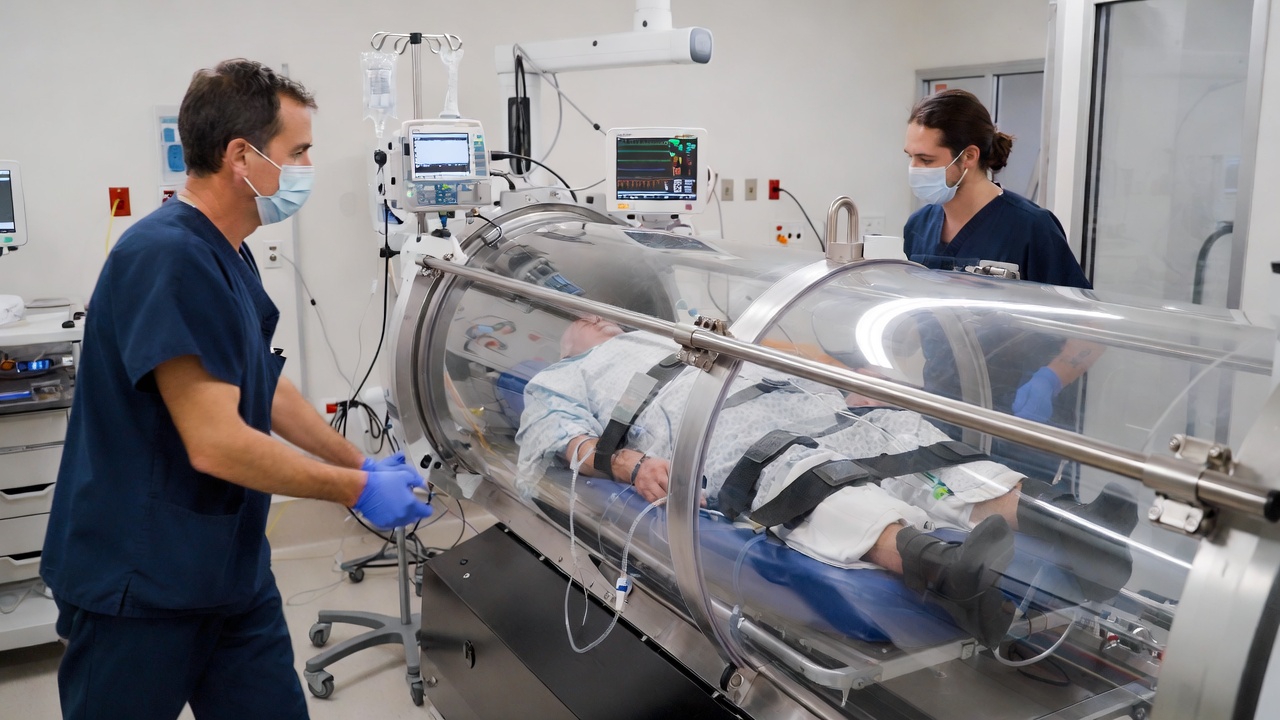
Monoplace chambers are built for one person. The patient lies inside a clear acrylic tube about seven feet long. The entire chamber is pressurized with pure oxygen. These are the most common hyperbaric chambers in independent clinics and smaller hospitals.
Multiplace chambers are room-sized vessels that can hold 10 or more patients at the same time. Patients sit in chairs and breathe pure oxygen through masks or hoods while the hyperbaric chamber itself is pressurized with regular air. A medical technician rides inside the chamber with the patients. These large chambers are found in major hospitals and military facilities. They cost more to build and operate, but they allow medical staff to be physically present during treatment.
This is where nearly all the clinical research has been conducted. When you read a study about HBOT therapy for diabetic wounds or radiation injury, the researchers almost certainly used a hard-shell hyperbaric chamber at 2.0 ATA or higher.
What you should know about clinical hyperbaric chambers:
- Pressure range: 2.0–3.0 ATA, delivering up to 1,824 mmHg of additional oxygen partial pressure above normal
- Cost per session: $75–$200 at most clinics, though some markets charge $400–$650
- Session length: 60–120 minutes, typically 5 days per week
- Typical protocol: 20–40 sessions for most conditions
- Supervision: Medical staff monitor you throughout each session
- Prescription required for pressures above 1.5 ATA
Pros: Maximum therapeutic pressure. Strongest evidence base. Clinical supervision means emergencies are handled immediately. Insurance may cover FDA-approved conditions.
Cons: Expensive when paying out of pocket ($1,500–$8,000+ for a full course). Requires travel to a clinic. Scheduling can be hard — 40 sessions over 8 weeks means a big time commitment.
2. Home Soft-Shell Chambers (1.3–1.5 ATA)

Soft-shell hyperbaric chambers (also called mild hyperbaric oxygen therapy or mHBOT) are inflatable, zippered enclosures designed for home use. Sometimes called an at home hyperbaric chamber or oxygen chamber, they have become popular in the consumer wellness market, with prices ranging from $4,000 to $15,000 to purchase, plus $500–$2,000 per year for oxygen supply and maintenance.
Here is where you need to understand the pressure math.
A soft shell hyperbaric chamber runs at 1.3 ATA. Normal air pressure at sea level is 1.0 ATA (760 mmHg). A soft-shell adds about 230 mmHg of extra pressure. A clinical hard-shell chamber at 2.4 ATA adds about 1,824 mmHg.
That means a soft-shell chamber gives you roughly 13% of the extra pressure that a clinical chamber does. That is not a small difference — it is a huge gap.
Why does this matter? Most studies use pressures of 2.0 ATA or higher. Proof of health benefits at 1.3 ATA is very limited. In fact, 1.3 ATA is often used as the “sham” (placebo) pressure in HBOT trials.
The best example: the U.S. military tested HBOT for brain injuries. They found that 1.3 ATA was “no better than a placebo” for lasting symptoms after concussion. Both groups got better — the benefit may have come from the rest and routine, not the pressure.
Other considerations for soft-shell chambers:
- Safety: Fire risk exists when concentrating oxygen without clinical supervision or emergency protocols
- FDA status: The FDA has cleared soft-shell chambers only for altitude sickness — not for the conditions most buyers want to treat
- No medical oversight: You are operating a pressurized oxygen device alone in your home
- Ongoing costs: Oxygen concentrators need replacement filters, and the chamber fabric degrades over time
Pros: Convenient — use it at home on your schedule. No per-session clinic fees. Some users report subjective benefits from regular sessions.
Cons: Very limited proof at 1.3 ATA. Often used as placebo pressure in clinical trials. High upfront cost for unproven health benefits. No emergency help if something goes wrong.
3. LiveO2 Adaptive Contrast — A Different Approach

LiveO2 Adaptive Contrast is not a hyperbaric chamber. It works in a completely different way. You exercise while breathing through a mask that switches between oxygen-rich air and oxygen-reduced air. Each session takes 15 minutes.
This approach is built on two well-studied methods. Oxygen multi-step therapy was created by German physicist Manfred von Ardenne in the 1960s [26]. He showed that exercise plus extra oxygen gets more oxygen into your tissues than either one alone. Intermittent hypoxic-hyperoxic therapy (IHHT) — widely studied in Europe — switches between low-oxygen and high-oxygen breathing. This triggers the body’s natural stress response, improving how cells use oxygen.
Research from a different field backs this up. Dr. Shai Efrati’s team at Tel Aviv University found what they call the “Hyperoxic-Hypoxic Paradox” [14]. Even inside a pressurized chamber, his method cycles patients between pure oxygen (mask on) and chamber air (mask off) every 20 minutes. The body reads each oxygen drop as a signal to start healing (HIF-1α signaling). Efrati’s key finding: the change between oxygen states is the signal, not the oxygen level itself.
LiveO2 Adaptive Contrast uses the same cycling idea — at normal air pressure. No chamber required. Delivered through a home system with coaching support. No prescription. No clinic. No chamber.
Side-by-Side Comparison
| Feature | Clinical Hard-Shell | Home Soft-Shell | Adaptive Contrast (LiveO2) |
|---|---|---|---|
| Pressure | 2.0–3.0 ATA | 1.3–1.5 ATA | 1.0 ATA (ambient) |
| Mechanism | Pressurized oxygen | Pressurized oxygen | Hypoxic-hyperoxic cycling + exercise |
| Cost per session | $150–$600 | N/A (ownership) | N/A (ownership) |
| Purchase cost | N/A | $4,000–$15,000 | $3,995–$6,995 |
| Session time | 60–120 min | 60 min | 15 min |
| Exercise required | No | No | Yes |
| Location | Clinic / hospital | Home | Home |
| FDA evidence | Strong (approved uses) | Very limited | Based on IHHT research principles; no device-specific clinical trials |
| Supervision | Medical staff | None | Coaching + training |
Your choice depends on your condition, your budget, and how much evidence you require before investing. For FDA-approved conditions, clinical hard-shell chambers have by far the strongest track record. For general wellness, weigh the evidence carefully before spending thousands on any system.
The Real Cost of Hyperbaric Oxygen Therapy
Before you commit to HBOT, you need to understand the full financial picture. Most people underestimate the total cost by 50% or more. Understanding the hyperbaric oxygen therapy cost upfront protects you from surprises. Here is what treatment actually costs in 2026.
(independent to hospital)
treatment course
treatment at clinical rates
Clinic Session Costs
A single HBOT session costs $150 to $600 depending on your market, the type of chamber, and the facility. Independent clinics typically charge $150 to $300. Hospital-based programs charge $300 to $600 or more.
But one session is never enough. Most conditions require 20 to 40 sessions minimum. Your provider will likely recommend 3 to 5 sessions per week over 4 to 12 weeks.
What a Full Treatment Course Costs
At the average price of $390 per session, a standard 40-session treatment costs $15,600. At the high end, that jumps to $24,000. Many ongoing conditions need 40 or more sessions every year.
That puts the annual cost for regular HBOT users at $15,600 to $31,200+ at clinical rates. Over five years, you could spend $78,000 to $156,000 on clinic sessions alone.
Home Soft-Shell Chambers
Buying a home soft-shell chamber costs $4,000 to $15,000 upfront. Add $500 to $2,000 per year for oxygen concentrator supply, replacement filters, and maintenance. The total first-year cost runs $4,500 to $17,000.
Home chambers cost less over time than clinic visits. But remember: soft-shell chambers operate at only 1.3 ATA — the pressure used as a placebo in clinical trials. You may be paying less for a treatment with far less evidence behind it.
The “Temporary Benefits” Trap
Here is the cost detail most clinics won’t mention. For many off-label conditions, your progress may go away when treatment stops. If your symptoms come back after 40 sessions, you face a choice: stop and lose your gains, or keep paying forever.
This turns a one-time treatment cost into a perpetual expense. A therapy that costs $15,600 per year becomes a $78,000 commitment over five years — with no guarantee of lasting results.
The Time Commitment Most People Don’t Plan For
Cost is only half the equation. Each hyperbaric chamber session takes far longer than the treatment itself.
A typical hard-shell session runs 60 to 90 minutes. But the clock starts well before you lie down. The chamber needs to pressurize — usually 10 to 15 minutes. When the session ends, depressurization takes another 10 to 15 minutes. Add the drive to and from the clinic, check-in, changing, and waiting for your slot. A “90-minute session” easily becomes a 3-hour commitment.
Now multiply that. A standard protocol calls for 5 sessions per week for 4 to 8 weeks. That is 20 to 40 sessions. At 3 hours per visit, you are looking at 60 to 120 hours — the equivalent of 1.5 to 3 full work weeks spent in and around a hyperbaric chamber.
For many people, this is the real deal-breaker. Even if they can afford the cost, they cannot afford the time. Jobs, caregiving, travel distance — the schedule is why many patients start a course of hyperbaric treatments but never finish. In one clinical trial, only 57% of patients completed all 40 prescribed sessions [3]. A larger study of over 6,000 patients found the median course was just 29 sessions — well short of the 30 to 40 typically recommended [23].
Use our calculator below to see what treatment would cost for your specific condition.
HBOT Cost Calculator
Select your condition and adjust the session cost to see a personalized estimate.
This calculator provides rough estimates based on average session counts and costs reported in published clinical studies. Your actual cost will vary based on your provider, location, severity, and treatment response. It is not medical or financial advice. Sources are shown with each result.
Range: $150 – $600 per session
Will Insurance Cover Your Hyperbaric Therapy?
For the conditions most people search for — TBI, chronic fatigue, anti-aging, athletic recovery, Long COVID, Lyme disease — insurance coverage is effectively 0%.
That is not an exaggeration. It is the documented policy of every major U.S. insurer. Here is exactly what each one covers, what they require, and what you will actually pay.
for HBOT are denied
timeline
off-label conditions
Medicare Coverage (NCD 20.29)
Medicare covers hyperbaric oxygen therapy for 15 specific conditions. The list has not changed in years. If your condition is not on it, Medicare will not pay.
The most common covered use is diabetic foot ulcers. Even that comes with strict requirements:
- The wound must be Wagner grade III or higher
- Standard wound therapy must have failed for at least 30 days
- The patient must show no measurable improvement during that period
- Documentation must prove all three criteria
When Medicare does cover HBOT, the patient still pays 20% coinsurance. At $300 per session for 40 sessions, that is $2,400 out of pocket even with coverage.
Getting Medicare to pay — even for approved conditions — is not easy. Claims need exact paperwork and the right codes. First-time denials are common.
The Prior Authorization Gauntlet
Even for covered conditions, insurers require prior authorization before treatment begins. Here is what that process looks like:
Off-Label Coverage: The Gut-Punch
If you are researching HBOT for any of these conditions, no major insurer will cover your treatment:
- Traumatic brain injury (TBI) — not covered
- Autism spectrum disorder — not covered
- Chronic fatigue syndrome — not covered
- Anti-aging and longevity — not covered
- Athletic recovery — not covered
- Long COVID — not covered
- Lyme disease — not covered
For these conditions, patients pay 100% out of pocket. A typical course of 40 sessions at an independent clinic costs $6,000 to $24,000. At hospital-based facilities, the same treatment runs $12,000 to $24,000+.
There is no payment plan that changes the math. Insurance will not help.
HSA and FSA Eligibility
HBOT qualifies for HSA and FSA spending when you have a letter of medical necessity from your doctor. Using pre-tax health savings provides an effective 25% to 35% discount depending on your tax bracket. It does not eliminate the cost — but it reduces the sting.
Risks, Side Effects & Safety
HBOT is generally safe when done at accredited facilities. But “generally safe” does not mean risk-free. Studies show a 29.81% overall side effects rate [15].
Most side effects are temporary. Some are not. Here is what the research documents.
Who Should NOT Get Hyperbaric Oxygen Therapy
HBOT is not safe for everyone. Certain medical conditions make pressurized oxygen dangerous. Before starting treatment, your provider should screen for all of the following:
- Untreated pneumothorax (collapsed lung) — This is an absolute contraindication. Pressure changes can make a collapsed lung life-threatening.
- Certain lung diseases — Severe COPD, emphysema with air trapping, or any condition that prevents air from escaping the lungs normally. Pressurization can cause serious complications.
- Active seizure disorders — If seizures are not well-controlled with medication, the added oxygen toxicity risk makes HBOT unsafe.
- Certain chemotherapy drugs — Bleomycin, cisplatin, and doxorubicin can interact with high-pressure oxygen and amplify their toxicity. Treatment timing matters — discuss this with your oncologist.
- Pregnancy — Generally avoided due to unknown effects on the fetus. The one exception is carbon monoxide poisoning, where the risk of not treating outweighs the risk of treatment.
- Recent ear or sinus surgery — Pressure changes can damage healing tissue or surgical repairs.
- Active upper respiratory infections — Congestion makes it difficult or impossible to equalize pressure, which can cause painful barotrauma.
Always disclose your full medical history to your provider before starting HBOT. This includes all medications, recent surgeries, and any history of lung problems, seizures, or claustrophobia.
Vision Changes
60% of HBOT patients experience temporary vision changes. The most common is myopic shift — a worsening of nearsightedness. This typically resolves 6 to 8 weeks after treatment ends. For patients over 50, existing lens conditions may be permanently affected.
Ear and Sinus Barotrauma
Pressure changes inside the chamber affect the ears and sinuses. 2% to 10% of patients experience barotrauma — pain, fluid buildup, or in rare cases, eardrum rupture. This is the most common acute side effect. Patients who cannot equalize pressure may need to stop treatment.
Oxygen Toxicity Seizures
Breathing pure oxygen at high pressure can trigger seizures. This is rare — roughly 1 in 3,400 sessions [13] — but it is serious. Seizures stop when oxygen delivery stops. Facilities must have trained staff and protocols ready for this event.
Claustrophobia
Monoplace chambers require lying inside a sealed tube for 60 to 90 minutes. 2% to 5% of patients drop out due to claustrophobia. This is not a medical risk, but it can make treatment impossible for some people.
Fire Hazard

This is the risk people underestimate the most. Inside a pressurized chamber, the oxygen level is much higher than normal. You are sitting inside a pressurized oxygen vessel. At these levels, things that don’t normally burn can catch fire fast. One spark can cause a flash fire in seconds.
At least 77 people have died in 35 documented hyperbaric chamber fires between 1923 and 1996 [24]. Every fatal fire occurred in an oxygen-enriched environment with flammable material present. Before 1980, most fires were caused by electrical faults. After 1980, the primary cause shifted to prohibited items brought into the chamber by patients — phones, lighters, electronics, and synthetic clothing. The FDA issued a formal safety communication in 2025 warning providers about fire risks during HBOT [25].
Still, many patients at wellness clinics bring phones, earbuds, and other electronics into the chamber. Some even post photos from inside on social media. This is extremely dangerous. A lithium battery failure, a static spark from earbuds, or a phone short circuit is all it takes.
Good hospitals have strict rules. Patients change into cotton gowns. Staff remove all personal items and check everything before sealing the chamber. Not all clinics follow the same standard.
If a facility allows you to bring your phone into the chamber, that should tell you something about their safety protocols.
Medication Interactions
Certain medications interact with hyperbaric oxygen. These include some chemotherapy drugs, topical wound products, and medications that affect blood sugar. Your doctor should review all medications before treatment begins.
FDA Warnings
The FDA has issued advisories against using HBOT for conditions it has not cleared. These warnings specifically address misleading marketing claims by some clinics and chamber sellers.
Soft-Shell Chamber Safety Concerns
Home soft-shell hyperbaric chambers are largely unregulated. Quality varies a lot between makers. These chambers have no medical staff, no emergency plans, and none of the safety features of hospital chambers. No standard safety certification exists for consumer soft-shell units.
What to Ask Your Doctor Before Starting HBOT
- Is HBOT FDA-approved for my specific condition?
- Will any of my current medications interact with hyperbaric oxygen?
- What is the facility’s accreditation status and safety record?
- What happens if I experience a seizure or barotrauma during treatment?
- What evidence supports the number of sessions being recommended to me?
Frequently Asked Questions
20–40 sessions is typical, but it depends on your condition. FDA-approved uses like diabetic wounds usually need 20–40 sessions at 2.0–2.4 ATA.
Off-label uses like TBI or concussion don’t have set guidelines. Some clinics suggest 40–80 sessions for brain conditions, but the proof behind those numbers is limited. Ask your provider to show you the research behind their treatment plan.
Generally safe, but not risk-free. Studies show a 29.81% side effects rate. The most common is temporary vision changes (about 60% of patients in longer treatments). Ear pain happens in 2–10% of patients.
Seizures are rare — about 1 in 3,400 sessions. Serious problems are uncommon when the rules are followed. See our full risks breakdown for details.
Soft-shell home chambers cost $4,000–$15,000. But they only reach 1.3 ATA — about 13% of the extra pressure you’d get in a clinic (2.0–3.0 ATA).
Almost all published research uses 2.0 ATA or higher. Proof of benefits at 1.3 ATA is very limited. Some studies even use 1.3 ATA as a placebo — meaning researchers don’t think it does much.
Clinical sessions run $150-$600 per visit. Home soft-shell chambers cost $4,000-$15,000 plus ongoing oxygen costs. A full 40-session clinical course typically totals $6,000-$24,000+. Insurance covers FDA-approved conditions at hospital-based facilities. Off-label use is almost always out-of-pocket. Use our cost calculator to estimate your total investment.
Three key differences. Pressure: Hard-shell chambers reach 2.0-3.0 ATA. Soft-shell chambers max out at 1.3 ATA — only 13% of the additional pressure. Evidence: Most published research uses hard-shell chambers at 2.0+ ATA. Very few studies test soft-shell pressures. Safety: Hard-shell chambers require trained operators and clinical supervision. Soft-shell chambers can be used at home but without medical oversight if something goes wrong.
Yes. LiveO2 Adaptive Contrast works in a completely different way than pressurized chambers. It is based on two well-studied methods: oxygen multi-step therapy (from the 1960s) and intermittent hypoxic-hyperoxic therapy (IHHT).
You exercise while the mask switches between oxygen-rich and oxygen-reduced air. This is designed to support your body’s natural adaptive response. Sessions take 15 minutes. No prescription needed. Designed for home use with coaching support. See our chamber comparison section for a side-by-side breakdown.
Start with four questions:
- Is your condition FDA-approved for HBOT? If yes, you have strong proof and possible insurance coverage.
- What’s your total budget — all sessions, travel, and time off work?
- Can you commit to 20–60 sessions over 4–12 weeks?
- What are your goals — treat something specific, or ongoing wellness?
Talk to your doctor first. Then watch our free webinar for step-by-step help.
A hyperbaric chamber is a sealed vessel that raises air pressure above normal levels. You breathe pure oxygen while inside the chamber. The extra pressure pushes more oxygen into your blood and tissues. Clinical hyperbaric chambers in hospitals reach 2.0 to 3.0 ATA. Some are monoplace chambers built for one person. Others are multiplace chambers that can hold 10 or more patients at once. Home soft shell hyperbaric chambers reach only 1.3 ATA. The type of hyperbaric chamber determines how much oxygen your body actually receives.
The main hyperbaric chamber benefits depend on the condition being treated. For FDA-approved conditions like diabetic wounds and radiation injury, HBOT therapy speeds healing by flooding damaged tissue with oxygen. Research shows it promotes new blood vessel growth, mobilizes stem cells, and reduces swelling. For off-label uses like brain injuries and anti-aging, evidence is still limited. See our FDA vs off-label breakdown for what the science actually supports.
It depends on the condition. Wound healing: Visible improvement often begins around sessions 10–15, as new blood vessels start forming in damaged tissue.
Neurological conditions like TBI and stroke recovery tend to take longer. Many patients report noticeable changes after 20–30 sessions, with full protocols typically running 40–60 sessions.
Off-label uses vary widely. Some people notice improvements within a few weeks. Others need the full course before seeing meaningful changes.
Individual responses differ significantly. Your age, the severity of your condition, overall health, and the pressure protocol used all affect the timeline. Your provider should set realistic expectations based on your specific situation — be cautious of anyone who promises fast results for complex conditions.
Start by looking for UHMS-accredited facilities (Undersea and Hyperbaric Medical Society). UHMS accreditation means the facility meets established safety and quality standards.
Hospital-based programs typically have the highest safety standards and most experienced staff. They also tend to have better emergency protocols if something goes wrong during treatment.
Questions to ask any facility:
- What ATA pressure do you use for my condition?
- How many sessions do you recommend, and what evidence supports that number?
- What is your safety record?
- Is a physician on-site during treatment?
Red flags to watch for: Clinics that promise guaranteed results for off-label conditions. Facilities without physician oversight. Pressure to buy large session packages upfront before you have tried even one session. Any facility that allows electronics inside the chamber.
For those considering home alternatives, see our chamber comparison section above.
HBOT Isn’t Your Only Option
There are faster, more affordable alternatives that use the same science. Watch this 4-minute preview, then register below for the full 15-minute webinar.
▶ 4-Minute Preview
Ready for the full picture? Here’s what the 15-minute webinar covers:
- Why pressure is only half the equation
- A comparison that could save you tens of thousands
- Why some people prefer training at home to $250/session clinics
- How alternatives compare to traditional HBOT — and what the research shows
- How to know if hyperbaric is right for your situation
15 min · Free · Watch instantly
Please enter your name and email to watch the webinar.
References
- Weaver LK, Hopkins RO, Chan KJ, et al. “Hyperbaric Oxygen for Acute Carbon Monoxide Poisoning.” N Engl J Med. 2002;347(14):1057-1067.
- Cifu DX, Walker WC, West SL, et al. “Hyperbaric Oxygen for Blast-Related Postconcussion Syndrome: Three-Month Outcomes.” Ann Neurol. 2014;75(2):277-286. (BIMA Trial)
- Löndahl M, Katzman P, Nilsson A, Hammarlund C. “Hyperbaric Oxygen Therapy Facilitates Healing of Chronic Foot Ulcers in Patients With Diabetes.” Diabetes Care. 2010;33(5):998-1003.
- Efrati S, Fishlev G, Bechor Y, et al. “Hyperbaric Oxygen Induces Late Neuroplasticity in Post Stroke Patients — Randomized, Prospective Trial.” PLoS ONE. 2013;8(1):e53716.
- Efrati S, Golan H, Bechor Y, et al. “Hyperbaric Oxygen Therapy Can Diminish Fibromyalgia Syndrome.” PLoS ONE. 2015;10(5):e0127012.
- Hachmo Y, Hadanny A, Abu Hamed R, et al. “Hyperbaric Oxygen Therapy Increases Telomere Length and Decreases Immunosenescence in Isolated Blood Cells.” Aging. 2020;12(22):22445-22456.
- Zilberman-Itskovich S, et al. “Hyperbaric oxygen therapy improves neurocognitive functions and symptoms of post-COVID condition: randomized controlled trial.” Sci Rep. 2022;12:11252.
- Rossignol DA, Rossignol LW, Smith S, et al. “Hyperbaric Treatment for Children with Autism: A Multicenter, Randomized, Double-Blind, Controlled Trial.” BMC Pediatr. 2009;9:21.
- Kranke P, Bennett MH, Martyn-St James M, Schnabel A, Debus SE, Weibel S. “Hyperbaric Oxygen Therapy for Chronic Wounds.” Cochrane Database Syst Rev. 2015;(6):CD004123.
- Moon RE. “Hyperbaric Oxygen Therapy Indications.” 14th Edition. Undersea and Hyperbaric Medical Society. 2019.
- Bouachour G, Cronier P, Gouello JP, Toulemonde JL, Talha A, Alquier P. “Hyperbaric Oxygen Therapy in the Management of Crush Injuries.” J Trauma. 1996;41(2):333-339.
- Cianci P, Slade JB Jr, Sato RM, Faulkner J. “Adjunctive Hyperbaric Oxygen Therapy in the Treatment of Thermal Burns.” J Burn Care Rehabil. 1994;15(5):408-415.
- Hampson NB, Atik D. “Central Nervous System Oxygen Toxicity During Routine Hyperbaric Oxygen Therapy.” Undersea Hyperb Med. 2003;30(2):147-153.
- Hadanny A, Efrati S. “The Hyperoxic-Hypoxic Paradox.” Biomolecules. 2020;10(6):958.
- Plafki C, Peters P, Almeling M, Welslau W, Busch R. “Complications and Side Effects of Hyperbaric Oxygen Therapy.” Aviat Space Environ Med. 2000;71(2):119-124.
- Hadanny A, Zubari T, Tamir-Adler L, et al. “Hyperbaric Oxygen Therapy Effects on Pulmonary Functions.” BMC Pulm Med. 2019;19:148.
- Gill AL, Bell CNA. “Hyperbaric Oxygen: Its Uses, Mechanisms of Action and Outcomes.” QJM. 2004;97(7):385-395.
- Hadanny A, Daniel-Kotovsky M, Suzin G, et al. “Cognitive Enhancement of Healthy Older Adults Using Hyperbaric Oxygen: A Randomized Controlled Trial.” Aging. 2020;12(13):13740-13761.
- Thom SR, Bhopale VM, Velazquez OC, et al. “Stem Cell Mobilization by Hyperbaric Oxygen.” Am J Physiol Heart Circ Physiol. 2006;290(4):H1378-H1386.
- Akarsu S, Tekin L, Ay H, et al. “The Efficacy of Hyperbaric Oxygen Therapy in the Management of Chronic Fatigue Syndrome.” Undersea Hyperb Med. 2013;40(2):197-200.
- Lin G, Zhao L, Lin J, Li X, Xu L. “Clinical Evidence of Hyperbaric Oxygen Therapy for Alzheimer’s Disease: A Systematic Review and Meta-Analysis of Randomized Controlled Trials.” Front Aging Neurosci. 2024;16:1360148.
- Bennett MH, French C, Schnabel A, Wasiak J, Kranke P, Weibel S. “Normobaric and Hyperbaric Oxygen Therapy for the Treatment and Prevention of Migraine and Cluster Headache.” Cochrane Database Syst Rev. 2015;(12):CD005219.
- Margolis DJ, Gupta J, Hoffstad O, et al. “Lack of Effectiveness of Hyperbaric Oxygen Therapy for the Treatment of Diabetic Foot Ulcer and the Prevention of Amputation.” Diabetes Care. 2013;36(7):1961–1966.
- Sheffield PJ, Desautels DA. “Hyperbaric and Hypobaric Chamber Fires: A 73-Year Analysis.” Undersea & Hyperbaric Medicine. 1997;24(3):153–164.
- U.S. Food and Drug Administration. “Follow Instructions for Safe Use of Hyperbaric Oxygen Therapy Devices — Letter to Health Care Providers.” FDA.gov. August 25, 2025.
- von Ardenne M. Oxygen Multistep Therapy: Physiological and Technical Foundations. Georg Thieme Verlag, Stuttgart. 1990.

